Socio-demographic characteristics
A total of 463 patients were recruited and 441 of them were included in the final analysis. The median length of hospital stay (LOS) was 6 days (95% CI: 6, 7) days. Two hundred twenty-five (51%) of the patients was in the age group of 41-60years old and more than two-fourth 230 (52.1%) of patients were male. Two hundred twenty-six (50.7%) of study participants were in the rural dwellers (Table 1).
Comorbidities asd patient related characteristics
About 56 (12.7%) patients have Diabetes Mellitus, while 44 (10%) patients have HIV/AIDS. The majority of patients (85.6%) do not drink alcohol. Nearly nine-tenths of participants (89.4%) were Never smokers while only about 17 (3.9%) were Current Smokers (Table 2). The mean body mass index (BMI) was 22.34 ± 2.7 kg/m2, six patients (1.4%) with BMI > = 30 Kg/m2. Seventy-one (16%) of patients reported as having a history of previous surgery and 38 (8.8%) patients were given a pre-operative blood transfusion. The majority, 344 (78%) were Clean-contaminated and, of those 40.4%, 26.4% and 1.4% of participants were belongs to ASA score I II, and IV respectively. Antibiotic Prophylaxis was given for 428 (97%) patients and of those, (83.5%) were given 30 min before the surgery. Drainage was inserted for 23 (5.2. %) of procedures and wound care was performed for 402 (91.1%) of post-operative patients (Table 2).
Type of surgical procedures
Large Bowel Surgery 176 (39.9%) was the leading procedure followed by other abdominal Procedures 87 (19.7%), Appendix surgery 61 (13.8%), Gastric Surgery 43 (9.7%), Gallbladder surgery 32 (7.2%), Herniorrhaphy 22 (5.0%), and Breast surgery 20 (4.5%)Incidence of SSI.
One hundred seventy-five patients (39.6%) developed surgical site infections (SSI). Among them, 128 cases (73.1%) were superficial SSIs, 42 cases (24%) were deep soft tissue SSIs, and 5 cases (2.9%) were organ/space SSIs.
We included 14 candidate prognostic predictors from the bivariable analysis into the initial multivariable model. After refinement, key prognostic predictors such as age, sex, wound care, wound class, ASA score, diabetes mellitus (DM), alcohol consumption, residence, preoperative hospital stay, and duration of surgery remained in the reduced model. Based on the results of this reduced model, we developed a prediction model and a corresponding nomogram (Table 3).
Model discrimination and calibration
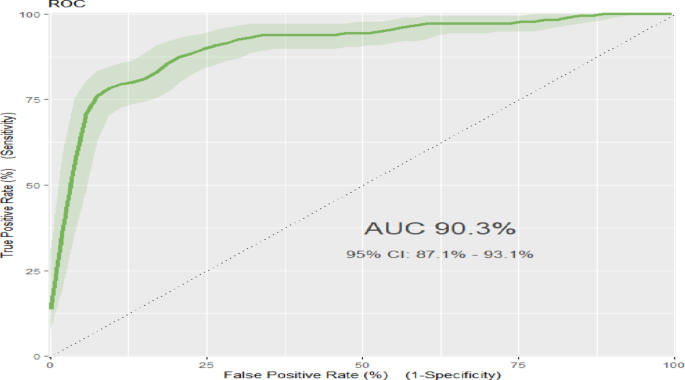
The area under the receiver operating characteristics curve (AUC) of the original model was 90.3% with 95% confidence interval of (87.1% to 93.1) (Fig). Based on the default 0.5 cut off probability, the original model has accuracy (ACC) of 90.3% with sensitivity (S) 0.78, specificity (SP) 0.90, positive predictive value (PV+) 0.83, and negative predictive value (PV-) 0.86(Fig. 1). However, based on the optimal cut of point (Youden index), 0.51 probability, the model has accuracy (ACC) of 0.87% with 95% CI (0.82.0.88), sensitivity(S) 0.78,95%CI (0.71, 0.84), specificity (SP) 0.90,95% CI (0.86, 0.93), positive predictive value (PV+) 0.83,95%CI (0.77, 0.89), and negative predictive value (PV-) 0.86, 95%CI (0.81, 0.90). It appears that at a 0.5 cutoff, specificity is highest, and accuracy is maximized. Whereas, at 0.51 cutoff, corresponding to the Youden Index (a point that optimizes both sensitivity and specificity), provides balanced performance across sensitivity, specificity, accuracy, PPV, and NPV (Table 4).

Receiver operating characteristics curve for prediction model of the original model.
Model calibration
The calibration plot for the model indicated, predicted probabilities are quite close to the red line, meaning that the model’s predicted probabilities are generally well-calibrated across the range of observed probabilities. The model does a good job of matching predicted outcomes with actual outcomes. The p vale is 0.366; Therefore, given an excellent calibration, the model might perform well in a new sample (Fig. 2).

Calibration belt for the original model: predicted probability versus observed probability of SSI.
The density plot showed the distribution of predicted probabilities for developing surgical site infections (SSI) across 441 patients, with color coding for actual outcomes (ground truth). Red represents patients without SSI (negative cases, 60.3%), while blue represents patients with SSI (positive cases, 39.7%). The plot showed some overlap in the model, revealing, it isn’t 100% perfect (Fig. 3).

Prediction density plot for surgical site infection risk: probability threshold distribution (n = 441).
To avoid over-interpretation and minimize too optimistic results from the original model; we used a bootstrapping technique using rms package to validate our model. This study used 1000 bootstrap samples with replacement; the corrected AUC was 87%, 95%CI (84%, 91%) and the optimism coefficient for the validated model was 0.0856. The β coefficients of the bootstrapped model were almost the same as the original β coefficients.
The calibration plot for the validated model indicated predicted probabilities are quite close to the observed probabilities. The calibration curve is close to the ideal line, indicates that the model is well-calibrated and performs reliably across different risk levels, predicting the probability of SSI accurately. A well-calibrated model, as suggested by this plot, means that the predicted probabilities (from the nomogram) correspond well with the actual probabilities observed in the dataset, making it a potentially useful tool for clinical decision-making (Fig. 4).

Calibration plot of the validated model: predicted probability versus actual probability of SSI.
Model summery
These ratios indicate that after optimism correction, the model retains about 82.6% of its original Dxy value and about 61.2% of its original R² value, suggesting a moderate degree of optimism bias, especially in the R2 metric.
|
Index. orig |
Training |
Test |
Optimism |
Index. corrected |
|
|---|---|---|---|---|---|
|
Dxy |
0.4922 |
0.5403 |
0.4546 |
0.0856 |
0.4065 |
|
R2 |
0.2268 |
0.2736 |
0.1855 |
0.0881 |
0.1387 |
Decision curve
The model has a higher standardized net benefit across a range of risk thresholds. The findings indicate that the model provides the best balance of benefit versus harm within the threshold range of approximately 0.1 to 0.6, after which its net benefit declines. For clinical or decision-making purposes, this model would be most useful within this risk threshold range. This implies that our model has the highest clinical and public health importance. Therefore, decisions made using the model such as safely discharging patients with some medications or keeping them for more intensive care in the hospitals has a higher net benefit (Fig. 5).

A plot of decision curve showing the net benefit of the model against threshold probability and corresponding cost-benefit ratio of SSI.
Simplified nomogram development for SSIs
A nomogram is a graphical calculating device or chart that represents a mathematical relationship between independent with the outcome variables. It is often used in medical fields to predict the probability of a particular outcome based on several predictor variables. It allows clinicians or decision makers to quickly estimate the risk or prognosis for individual patients without needing complex statistical calculations. The nomogram was developed from: sex, age, preoperative hospital stays, history of surgery, duration of surgery, alcohol consumption, residence, DM, ASA, wound care, and wound class. It consists of elven parallel lines or scales that represent different predictor variables. Each variable is assigned a point value, and the total risk is estimated by summing these points and referring to a final scale. To use this nomogram, a clinician or user plots the value of each predictor variable on the respective scales (top point scale), sums the points, and then reads the corresponding risk estimate from a final scale (total points scale), then read down to the SSI (Fig. 6).

Nomogram for predicting the probability of developing surgical site infections (SSIs).
For example, if patient is male, wound care, and ASA, the point for each variable is 49, 75, and 100 respectively. when we sum up the result is 224, then we go down to the total pint scale and point the result to SSI (probability of the outcome) and point on the scale. Therefore, for the above variable the probability of SSI is 0.6 (60%). To predict an individual estimated risk of SSI from patients who undergone surgery based on linear predictors of validated regression coefficients as: the probability of SSI = 1/1 + exp-(-17.25 + 1.46*sex + 0.36*residence + 6.92*age1 + 0.15*age2 + 6.4*age3 + 1.84*preoperative hospital stay + -0.84*duration of surgery + 1.34*history of surgery +-0.12*alcohol + 1.04*DM + 3.07*ASA+-0.49*wound class+-2.24*wound care.
link