Study selection results
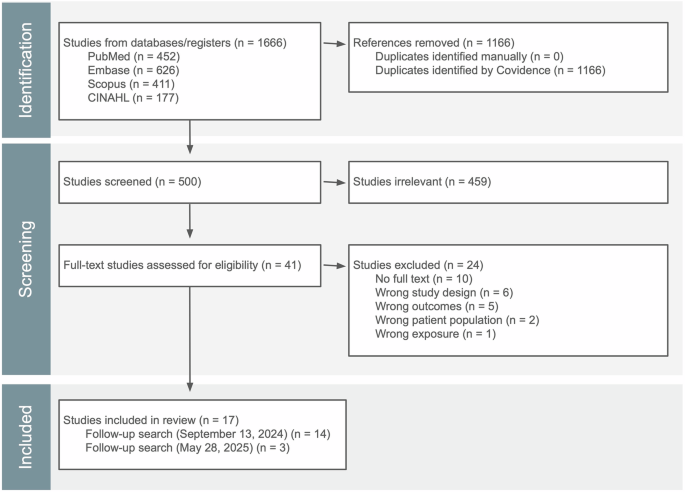
The initial search on September 13, 2024, yielded 683 publications. To ensure comprehensiveness, the search strategy was expanded to include additional keywords, and a final search was conducted on May 28, 2025, yielding 983 records (Supplementary Table 1). The publications were imported to Covidence for screening, resulting in 500 unique studies after removing duplicates (Fig. 1). Of these, 41 full texts were screened for eligibility, and seventeen studies were ultimately included in this review. A summary of findings for the included studies is presented in Table 1, and Supplementary Table 2 lists the excluded articles along with the reasons for exclusion.
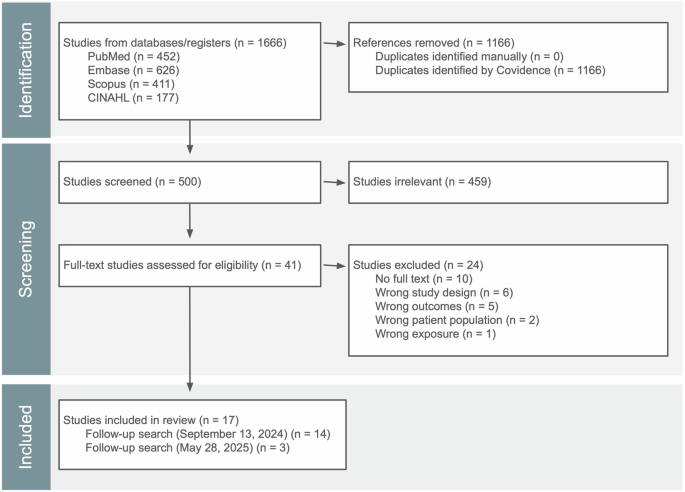
This PRISMA flow diagram summarizes the number of records identified through the database search, screened for eligibility, and included in this systematic review.
Quality assessment
Using the modified Oxford Centre for Evidence-based Medicine (OCEBM) rating scheme, eight of the 17 studies in this review have a quality rating of three, and nine have ratings of four (Table 1), reflecting their retrospective cohort and cross-sectional study designs16,17. The Grading of Recommendations, Assessment, Development, and Evaluations (GRADE) method showed that quality was low to moderate overall (Table 2), mainly due to the observational nature of these studies as well as inconsistencies in what population characteristics the studies used to proxy LEP18.
Study characteristics
Among the 17 studies included, nine used a cross-sectional study design and eight employed a retrospective cohort study design. Sample sizes ranged from n = 718 to n = 1,241,313. Studies were conducted in the northeast U.S. (n = 2), California (n = 8), Oregon (n = 1), Washington (n = 1), Wisconsin (n = 1), Illinois (n = 1), Minnesota (n = 1), and nationally (n = 2). Five studies used survey data, and 12 used electronic health records. Studies also spanned different fields of medicine, including primary care (n = 4), contraceptive care (n = 1), cardiology (n = 1), rheumatology (n = 1), oncology (n = 2), and general/multispecialty (n = 8). All studies looked at the ambulatory setting.
These 17 studies were grouped into three review categories of telemedicine use for patients with LEP: 1) overall utilization of telemedicine, 2) utilization of telemedicine compared to in-person visits, and 3) utilization of video- versus telephone-based telemedicine. Among the included studies, 41% (7/17) reported on telemedicine utilization frequency in the last 12 months or during the study period, 41% (7/17) reported on telemedicine utilization compared to in-person visits, and 41% (7/17) reported on video utilization compared to telephone use for telemedicine visits. Three studies reported on more than one of the three categories.
Outcome 1: Overall telemedicine utilization
Even though telemedicine has emerged as a critical component of healthcare delivery, disparities in its access and utilization persist, particularly among patients with LEP. Five of the seven studies reviewed in this section found significantly lower telemedicine utilization for patients with LEP compared to those with EP19,20,21,22,23. One study showed no difference in telemedicine utilization between two populations24. One study showed significantly higher telemedicine utilization for patients with LEP25.
Three survey studies investigating various care settings found lower telemedicine usage by LEP patients than by EP patients. Using National Health Interview Surveys data on nonelderly adults, Chang et al. reported a significantly lower percentage of patients with LEP having any telemedicine visits compared to those with EP21. After adjusting for enabling, predisposing, and need factors, LEP patients had 20% lower odds of having a telemedicine visit compared to EP patients (aOR, 0.80; 95% CI, 0.66–0.96; p = 0.02)21. Analysis of the 2015-2018 California Health Interview Survey (CHIS) data also found lower rates of telemedicine use by patients with LEP compared to EP speakers (4.8% vs. 12.3%)20. A later study using the 2021 CHIS adult data similarly found that patients with LEP were less likely to report using telemedicine (video or telephone) compared to patients with EP (OR, 0.63; 95% CI, 0.52–0.77; p < 0.001)19.
A similar negative association was seen in a rheumatology setting in Washington state. Thomason et al. reported that patients who preferred Spanish or other non-English languages were less likely to use video-based visits than patients who preferred English (Spanish OR, 0.27; 95% CI, 0.15–0.47; p < 0.001; other non-English languages OR, 0.34; 95% CI, 0.21–0.55; p < 0.001)22.
Lower telemedicine usage by LEP patients compared to EP patients was seen in oncology, as well as in a study looking at patients in a California cancer center. Azizi et al. found that patients with Spanish- and Vietnamese-preferences were both less likely to have had virtual visits than EP patients (Spanish: mean difference: −5%, p < 0.001; Vietnamese: mean difference: −5%, p < 0.001)23.
In contrast to the statistically significant lower LEP patient telemedicine use in the studies above, one study analyzing telemedicine utilization stratified ethnic groups by Chinese and Latino populations in California and found no significant difference between LEP and EP groups. This study, conducted by Gordon et al., examined patients with at least one outpatient visit in the first nine months of the COVID-19 pandemic and reported a similar prevalence of virtual care use between LEP and EP patients for both Chinese and Latino groups24.
One cross-sectional study conducted via survey, looking at counties across the U.S. falling under the highest and lowest quartiles of the Minority Health Social Vulnerability Index, reported that those with LEP had higher adjusted odds of utilizing telemedicine25. Patients with LEP in these quartiles had 1.6 times the odds of non-emergency room-related video or phone visits compared to those with EP (aOR, 1.60; 95% CI, 1.28–1.99)25.
Outcome 2: Telemedicine utilization compared to in-person visits
In addition to the studies investigating overall telemedicine utilization, seven studies directly compared telemedicine use to in-person visits. Five of the seven studies reported lower odds of telemedicine utilization for LEP patients7,26,27,28,29. One study reported opposite patterns of telemedicine utilization depending on interpreter use30, while another observed slightly higher telemedicine usage among LEP patients31.
For ambulatory clinics in Oregon, Sachs et al. found that patients who preferred Spanish or other non-English languages had lower odds of using telemedicine compared to EP individuals (Spanish OR, 0.63; 95% CI, 0.59–0.69; p < 0.001; Other non-English OR, 0.20; 95% CI, 0.17–0.23; p < 0.001)26. Similar negative associations between telemedicine utilization and LEP were reported by Osmanlliu et al. in California. For adult cardiovascular ambulatory care, patients with non-English language preferences had lower odds of telemedicine visits (OR, 0.80; 95% CI, 0.72–0.88)7. A study on contraceptive healthcare services in California by Meurice et al. also showed that patients with Spanish language preference had significantly lower adjusted odds of choosing telemedicine over in-person care (OR, 0.53; 95% CI, 0.44–0.64; p < 0.001)27.
Similarly, a lower utilization of virtual visits vs. in-person visits by patients with LEP compared to EP was reported for clinical pharmacist visits in a family medicine clinic in Minnesota29. LEP patients had 11.2% fewer virtual visits compared to EP patients (absolute difference: −11.2%; p < 0.001)29.
A study by Tong et al. in an oncology facility in Wisconsin found that patients needing interpreter services had significantly lower odds of using telemedicine compared to in-person visits (OR, 0.4; 95% CI, 0.30–0.52; p < 0.001)28. Unlike previous studies, which used language preference to classify LEP or EP, this study defined patients with LEP as those documented as requiring an interpreter.
While the previous studies showed consistently lower telemedicine utilization compared to in-person visits for patients with LEP, one study by Parameswaran et al. reported an opposite association of telemedicine utilization when looking at LEP defined by either language preference or interpreter need30. This study, conducted at a large academic medical center in California, investigated primary care telemedicine visits for new and returning patient visits. For new patient visits with patients with Spanish and Mandarin language preferences, there was a significantly lower utilization of telemedicine compared to in-person visits for both language groups (Spanish OR, 0.60; 95% CI, 0.44–0.81; Mandarin OR, 0.74; 95% CI, 0.56–0.98). For returning patient visits, a significantly lower telemedicine utilization was seen only for Spanish preference (Spanish OR, 0.70; 95% CI, 0.63–0.77; Mandarin OR, 1.04; 95% CI, 0.95–1.14). However, when looking at interpreter service use rather than language preference, a significantly greater utilization of telemedicine was found for both new (OR, 1.83; 95% CI, 1.41–2.38) and returning patient visits (OR, 1.19; 95% CI, 1.10–1.28)30.
In contrast to most of the other studies, one study found that patients with non-English preference had slightly higher adjusted odds of using telemedicine over in-person participation31. Zachrison et al. examined ambulatory care visits in a large New England healthcare system and found slightly higher adjusted odds for patients with a non-English language preference (aOR, 1.034; 95% CI, 1.01–1.06; COVID-19 timeframe: aOR, 1.05; 95% CI, 1.03–1.08). This study noted that the different trend may have reflected, at least partially, their pre-pandemic adoption of telemedicine and better health system preparedness31.
Outcome 3: Video compared to telephone use for telemedicine
Seven studies investigated differences in telemedicine utilization by modality, video versus telephone, among patients with LEP. All the studies showed significantly less video use by patients with LEP compared to patients with EP7,24,26,31,32,33,34. One study reported that while LEP was associated with lower use of video than audio, for the subset of patients with prior experience with video visits, there was no difference in visit modality between patients with LEP compared to EP32.
A study by Yoon et al. involving patients with chronic conditions at higher risk for COVID-19 from a group of academic and community health centers in Illinois showed that patients with LEP had significantly lower odds of using video for telemedicine visits compared to those with EP (OR, 0.36; 95% CI, 0.13–0.95)33. Similarly, a large academic health system in the Pennsylvania and New Jersey area found that LEP patients had lower adjusted odds of utilizing video for telemedicine visits in the primary care setting (OR, 0.85; 95% CI, 0.76–0.95)34. A similar negative association was seen for LEP video visits for primary and specialty ambulatory care at another Northeast hospital system (OR: 0.89; 95% CI, 0.86–0.93)31. A study by Osmanlliu et al. in a cardiovascular ambulatory care setting in Northern California found that LEP patients were less likely to use video visits compared to telephone visits (OR, 0.52; 95% CI, 0.46–0.59)7.
Sachs et al.’s study at ambulatory clinics in Oregon looked at patients who preferred Spanish and other non-English languages. Both LEP groups had lower odds of using video visits than EP patients, with a stronger association for those preferring Spanish (Spanish OR, 0.20; 95% CI, 0.17–0.23; p < 0.001; other non-English OR, 0.41; 95% CI, 0.25–0.48; p < 0.001)26.
Gordon et al.’s study on primary and specialty healthcare in California looked at two ethnic groups and compared LEP and EP patients within each group. It was also concluded that, within the same age strata, LEP adults were more likely to use phone visits and less likely to use video visits than EP adults for both Latino and Chinese populations24.
Studies that defined LEP as the need for interpreters reported a similar negative association. Hsueh et al.’s study on primary care visits in California found that LEP individuals were significantly less likely to use video-based visits compared to EP patients, and often defaulted to telephone-only consultations (OR, 0.77; 95% CI, 0.74–0.80)32. However, further analysis showed that among patients with prior video visit experience, there was not a significant difference between LEP patients’ and EP patients’ likelihood of choosing the video visit modality (47.2% vs 49.1%; p = 0.09).
link